10 Mar Why Varicose Veins Are More Than Just a Cosmetic Issue
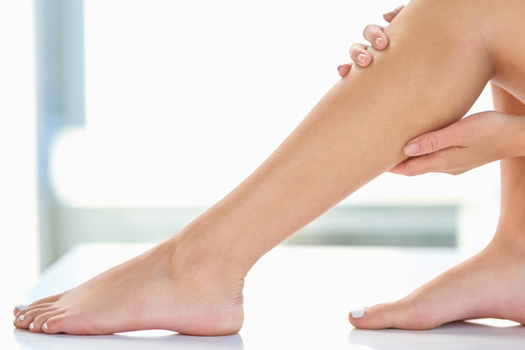
Varicose veins present as enlarged, twisted blood vessels, and they typically appear on the legs or feet. Some individuals may view these visible veins as a cosmetic concern, but they actually indicate an underlying medical condition. This condition involves blood flow and requires careful medical evaluation. Understanding the nature of this venous issue helps patients make informed decisions about their health.
What Are Varicose Veins?
Varicose veins are swollen blood vessels that bulge just beneath the surface of the skin. They most commonly occur in the lower extremities, and they often appear blue or dark purple. Healthy veins push blood toward the heart, but varicose veins struggle to do so due to internal changes. Blood subsequently pools within the vessel, creating the characteristic enlarged appearance.
What Causes Them?
Veins contain one-way valves that prevent blood from flowing backward. These internal valves can weaken over time or sustain damage from various factors. When the valves fail to function correctly, blood begins to accumulate in the vein. The vein then stretches from the increased pressure, and this structural change leads to varicosity.
Several risk factors contribute to the development of this venous condition. Advancing age naturally causes wear and tear on the valves, and a family history of venous disease increases the likelihood of occurrence. Pregnancy also places additional strain on the circulatory system. Excess body weight creates additional pressure on the legs, so managing weight helps mitigate the risk.
What Are the Symptoms?
Patients with varicose veins experience a range of physical symptoms beyond the visual changes. The affected legs often feel heavy, and a dull ache may develop after prolonged periods of standing. Muscle cramping may occur during the night, with patients noticing swelling around their ankles. Some individuals experience throbbing pain or an uncomfortable itching sensation around the specific veins.
What Are the Treatment Options?
Medical advancements provide several minimally invasive methods for addressing varicose veins. Doctors often recommend endovenous ablation, a procedure that uses laser or radiofrequency energy to close off the affected vein. The body eventually absorbs the closed vein, and blood naturally reroutes through healthier blood vessels. This approach requires minimal recovery time, so patients can resume normal activities relatively quickly.
Another available treatment option is Varithena®, which uses a specialized microfoam. The physician injects this foam directly into the diseased vein, which causes the vein to collapse. VenaSeal® vein treatment offers a different approach by delivering a small amount of medical adhesive to close the vein. The adhesive seals the vessel shut, and the redirected blood flow relieves the associated symptoms.
How Is Professional Care Beneficial?
Seeking guidance from a vascular specialist can help patients obtain a diagnosis. A medical professional will evaluate the severity of the condition, and they may use ultrasound imaging to map the venous system. This assessment identifies the root cause of blood pooling. The specialist then develops a targeted treatment plan, helping patients achieve effective results.
Attempting to manage the condition without medical supervision may lead to progressive complications. The pooled blood can eventually cause venous ulcers, and these open sores require extensive wound care. Proactive medical treatment halts disease progression and restores proper circulatory function in the lower extremities.
Consult a Specialist Today
Varicose veins represent a distinct medical condition that requires proper clinical evaluation. The available treatments address both the symptoms and the underlying structural issues, so patients do not need to endure ongoing discomfort. Schedule an evaluation with a vein specialist today to improve your venous health.
- Senior Care Solutions for Independent Living: Helping Older Adults Live Safely and Comfortably
- Health and Wellness Methods for Emotional Balance: A Complete Guide to Inner Peace and Well-Being
- Comprehensive Cardiovascular and Orthopedic Care: A Complete Approach to Better Health
- How to Find the Best Dermatologist Near Me? A Complete Guide for Healthy Skin
- Crypto Investment Strategies for Beginners




No Comments