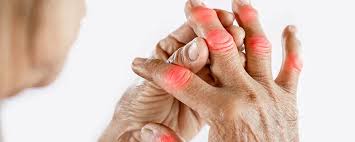
03 Apr When do Arthritis Symptoms Become Serious?
Arthritis symptoms change over time. Joint pain may happen, and stiffness often occurs. You experience flare-ups and mobility decreases when inflammation rises. Symptoms sometimes worsen, so reach out to your provider for support.
What warning signs require attention?
Joint pain is a common experience in arthritis. Severe pain can persist, and it requires careful observation. Stiffness sometimes worsens, and you lose motion if joints swell, making tasks like walking up stairs or gripping objects harder. These physical changes disrupt daily activities; you may have trouble with routine tasks like getting dressed or making meals. Symptoms affect your daily routine by limiting both large and small movements.
Redness and joint warmth appear as inflammation increases, signaling changes in joint health. Monitor these shifts, as changes can happen gradually or suddenly, and new symptoms should be discussed with your provider. Swelling is visible, and it also creates pressure or tightness in the joint. This makes even light movement uncomfortable.
What risk factors increase severity?
Certain factors influence arthritis progression. Aging wears down cartilage, and uric acid can cause gout by building up in the joints. Family history matters, and risks rise because genetics affect joint health and susceptibility to types. Previous joint injuries accelerate wear, so people with sports injuries or fractures can experience arthritis sooner than others. Obesity adds stress to joints because extra weight increases pressure, especially in weight-bearing joints like the hips and knees. Daily habits such as physical inactivity or poor nutritional choices influence how arthritis develops. Autoimmune diseases sometimes affect joint health, especially if you have other conditions that influence your immune system. The immune system sometimes malfunctions, and this affects healthy joints in conditions like rheumatoid or psoriatic arthritis.
What treatment options offer relief?
Medical Treatments Explained
Medical interventions help manage joint inflammation by using a personalized approach. Not every strategy works for all. Corticosteroids help reduce swelling, and physical therapy improves mobility. They teach you exercises to strengthen muscles supporting your joints. NSAIDs reduce pain and symptoms; these medications are available over-the-counter. DMARDs are sometimes used to treat rheumatoid arthritis by modifying the immune response. This can help manage progression. Medications can help address symptoms, and they support joint function. Splints support joints, and braces help while you move around by reducing stress on the affected area.
Practical Lifestyle Strategies
Providers tailor these treatments to your symptoms, so use open communication. They suggest adjustments if you have medical conditions affecting your treatment choices. Lifestyle changes support joint health as part of a holistic approach. Weight loss helps relieve joint stress, especially in the knees and hips. Dietary changes can address inflammation, so avoid processed foods. Include more fruits, vegetables, and omega-3-rich foods. Low-impact exercises such as swimming and biking give you options for exercise. These exercises can minimize joint strain.
Manage Your Arthritis Symptoms Today
Your health requires proactive management. Consult your provider, and discuss your current symptoms. Taking action prevents damage, and outcomes may improve when you seek help. Track your daily joint pain. Schedule an appointment for guidance. Since arthritis can affect daily life, treatments offer some comfort. Start your treatment plan today.




No Comments